Contact allergic dermatitis

IMPORTANT The information provided is of a general nature and should not be used as a substitute for professional advice. If you think you may suffer from an allergic or other disease that requires attention, you should discuss it with your family doctor. The content of the information articles and all illustrations on this website remains the intellectual property of Dr Raymond Mullins and cannot be reproduced without written permission.
Summary
Contact allergic dermatitis (contact dermatitis, contact eczema) describes the rash that develops after skin contact with external "allergens". Nickel, plants and perfumes are the most common triggers.
What is contact allergic dermatitis?
Contact allergic dermatitis (contact dermatitis) develops after skin contact with external "allergens". A red, itchy and often blistering weeping rash develops, typically within a few days of contact with external "allergens".
Timing is everything
Skin irritation, itch and redness may start within half to 5 days after exposure, but the average is 1 to 2 days. The rash then worsen over the next 2 to 3 days, and watery blisters are often noticed. Symptoms then settle over a period of 3 to 7 days, with involved skin becoming dry and rough, and often peeling.
What is happening?
The body's immune system recognizes allergen as "foreign". When this happens, white cells are attracted from the blood into the skin over several days. This results in inflammation and the development of a rash.
Common causes
Over 2000 contact allergens have been identified, of which nickel, plants and perfumes are the most common. Here are some of many:
NICKEL DERMATITIS. Around 1 % of the population is allergic to this metal, present in plated jewellery, watch buckles, jeans studs, keys, coins, bra clips, cooking utensils, gym equipment.
HAIR DYES.
RUBBER ADDITIVES. eg. gloves, rubber handled tools or gym equipment or bike handles.
FRAGRANCES. eg. perfume, shampoos, cosmetics, tissues, deodorants, domestic cleaners.
LEATHER ADDITIVES, TEXTILE DYES
FORMALDEHYDE. eg. permanent press clothes, cosmetic preservatives, glossy paper
COLOPHONY. This is a pine resin present in wood as well as pine oil cleaners and band aid gums
PLANTS. eg. grevillea, bulbs, daisies, dandelions, chrysanthemum, ivy, tomato plants, zucchini plants, garlic, onion, primrose, poison ivy, mango (often causes a rash around the mouth), Rhus trees, tea tree oil
COSMETICS / SUNSCREEN ADDITIVES. eg. PABA, oxybenzone, benzophenone
PLASTICS. eg methacrylates glues, dental plates and even Australian plastic bank notes!.
FLAVOURING AGENTS. eg. cinnamates in toothpastes or foods.
MEDICATION PRESERVATIVES. eg. benzylkonium chloride in eyedrops, lanolin in some creams, topical antibiotics or local anaesthetics (used to treat sting/bite reactions).
Sometimes light is needed too
So-called photo-contact dermatitis requires both contact with allergen and light exposure for a rash to develop.
The story is everything
Because the rash does not develop immediately, the story surrounding the episode is very important. This will help you and your doctor to identify the cause so that exposure can be avoided in the future. You may be asked to write down what you have done or come into contact with, in the previous few days.
-
•Were you in the garden?
-
•What plants do you have?
-
•What work do you do?
-
•Do you work with solvents or chemicals or gloves?
-
•What hobbies do you have?
-
•Did you change your shampoo or cosmetics?
-
•Did you have your hair dyed?
-
•Did you use any new creams or sunscreens?
-
•Were you outside in the last few days?
-
•Are you aware of anything that you already know causes rashes (like band aids, jewellery)?
-
•Are you using any new medication (tablets, eyedrops, creams etc)?
When to suspect contact allergic dermatitis
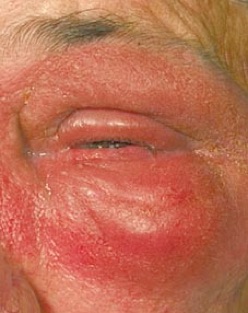
While there are no firm rules, one must be suspicious in some circumstances such as isolated face or eyelid dermatitis, hand dermatitis or the sudden onset of dermatitis in someone who has not had similar rashes before. Rashes involving only 1 or 2 body areas may also lead one to suspect a localised allergic cause.
Obvious contact with allergen is not always needed
Contact allergy can be direct. eg, makeup put on a face, indirect (eg. via the hands or a hug) or airborne. Contact with airborne perfumes or plant-derived allergen can also cause dermatitis. This is commonly known as "Australian bush dermatitis", ragweed dermatitis or weed dermatitis. Wind-blown allergen comes into contact with exposed areas of skin over the face, eyelids, sides of neck and "V" area of the neck and upper chest. Dermatitis often occurs after being outside on a windy days in the warmer months of the year. There is usually a sharp line between affected areas, and normal skin protected by clothing. Even lightly brushing past a plant can trigger dermatitis in someone very sensitive to it.
Allergy testing (Patch testing)
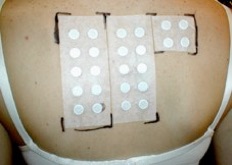
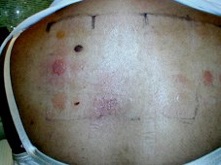
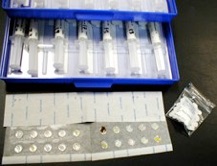
Skin prick testing is of no use in this condition. Instead, "Patch testing" is performed. Commercial allergen extracts are applied to marked areas of rash-free skin, usually over the back. Allergen extracts are applied using low allergen tape.and left in place for around 2 days. The results are then "read" over the next few days. The presence of a rash under an individual allergen indicates sensitivity to this substance. This does not prove that this particular allergen is the cause, but may provide a clue of what may be causing your problem.
How is contact dermatitis treated?
Antihistamines (such as Claratyne, Telfast, Zyrtec, Phenergan or Polaramine) are usually unhelpful in controlling itch or irritation. Mild rashes can be treated with cortisone / steroid creams to reduce inflammation. Severe blistering episodes usually require cortisone / steroid tablets for several days to control symptoms.
Last reviewed 19 June 2020
References
Devos SA, Van Der Valk PG. Epicutaneous patch testing. Eur J Dermatol. 2002 Sep-Oct;12(5):506-13. Review
Peate WE. Occupational skin disease. Am Fam Physician. 2002 Sep 15;66(6):1025-32. Review.
Basketter DA, Evans P, Gerberick GF, Kimber IA. Factors affecting thresholds in allergic contact dermatitis: safety and regulatory considerations. Contact Dermatitis. 2002 Jul;47(1):1-6. Review.
Smith HR, Basketter DA, McFadden JP. Irritant dermatitis, irritancy and its role in allergic contact dermatitis. Clin Exp Dermatol. 2002 Mar;27(2):138-46. Review.
Cook N, Freeman S. Report of 19 cases of photoallergic contact dermatitis to sunscreens seen at the Skin and Cancer Foundation. Australas J Dermatol. 2001 Nov;42(4):257-9. Review.
Koch P. Occupational contact dermatitis. Recognition and management. Am J Clin Dermatol. 2001;2(6):353-65. Review.
Scheinman PL. Exposing covert fragrance chemicals. Am J Contact Dermat. 2001 Dec;12(4):225-8. Review.
Holdiness MR. Contact dermatitis to topical drugs for glaucoma. Am J Contact Dermat. 2001 Dec;12(4):217-9. Review.
Kanerva L. Cross-reactions of multifunctional methacrylates and acrylates. Acta Odontol Scand. 2001 Oct;59(5):320-9. Review.
Carson CF, Riley TV. Safety, efficacy and provenance of tea tree (Melaleuca alternifolia) oil. Contact Dermatitis. 2001 Aug;45(2):65-7. Review.
Wolf R, Wolf D, Tuzun B, Tuzun Y. Contact dermatitis to cosmetics. Clin Dermatol. 2001 Jul-Aug;19(4):502-15. Review. No abstract available.
Koutis D, Freeman S. Allergic contact stomatitis caused by acrylic monomer in a denture. Australas J Dermatol. 2001 Aug;42(3):203-6. Review.
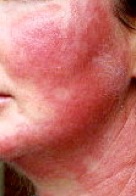
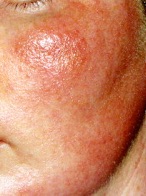
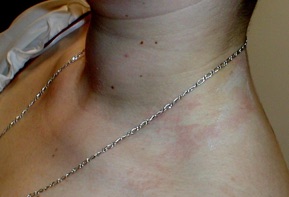
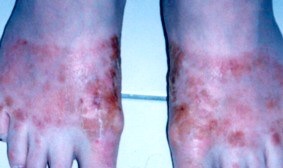
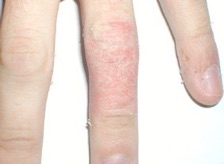
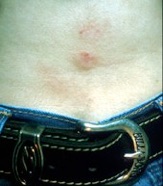


Contact dermatitis due to makeup, metal necklace, shoes, sticking plaster, metal jeans studs and a paint gun is shown above. Patch testing photos are shown below, performed on the back.